Young couples expecting twins have two times the delight of having a child. Eyo Etim Okon, a 39-year-old principal, is an exception. His wife had complications giving birth to twin boys, and eight days later she passed away. As a result, baby Asher, one of the twins, was in dire need of oxygen to treat his respiratory distress.
His breathing got difficult. I was concerned because I wondered what would happen to him if the oxygen ran out. All I can say is how happy I am that Calabar’s University Teaching Hospital has oxygen, added Eyo.
According to Dr. Glory Bassey, the Consultant Pediatrician at the University of Calabar Teaching Hospital, “The availability of oxygen itself is important first. Oxygen is life. The availability of oxygen itself is a challenge presently in this center. Parents buy oxygen but thank God for the intervention that is ongoing with the construction of the oxygen plant in this hospital. It is a welcome development.
Medical oxygen is a necessary and life-saving drug. It is essential for the treatment of critical respiratory and life-threatening illnesses such as severe pneumonia, severe malaria, sepsis (caused by bacteria and viruses), COVID-19, trauma, and difficulties during childbirth or pregnancy. It can be utilized at all levels of the healthcare system, and safe surgical, emergency, and critical care services must be provided.
The management of pneumonia and hypoxemia was taught to a few health professionals in Cross River to enhance the skills required for oxygen therapy in young children, especially newborns. The workshop aimed to scale back training in pediatric hypoxemia care and inpatient management of community-acquired pneumonia.
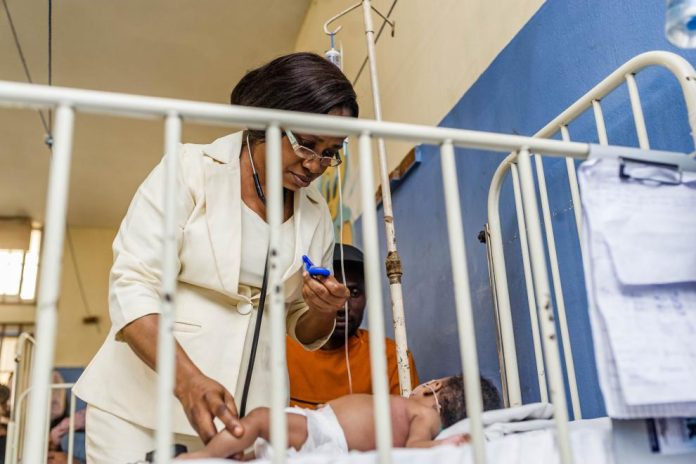
One of the health professionals who benefited from the step-down training was Esther Ese Onah, a pediatric nurse in charge of the Neonatal unit and the nurse in charge of baby Asher. According to Esther, the training has enabled her to successfully manage newborns who are experiencing respiratory distress. “The training has assisted me in detecting early a baby needing oxygen therapy, and I’m able to initiate treatment promptly utilizing an oxygen concentrator to help the child to breathe.”
“From the onset of admission, the baby (Asher) was monitored hourly, then every two hours. At this stage, we are happy with his respiratory rate. We check him every four hours. Hopefully, he will be discharged next week as his breathing improves,” added Esther.
Dr. Janet Ekpenyong, the Cross Rivers State Commissioner for Health, asserts that the significance of oxygen cannot be overstated. “You will agree with me that the high mortality rate globally or even in Nigeria is a result of poor oxygen or non-availability of oxygen. I tell you most of the deaths would have been prevented if all facilities had oxygen,” she said.
“We are happy to have a newly constructed oxygen plant in Cross Rivers. It will serve all the primary and secondary facilities in the state. We are committed to ensuring we have the human resources needed and electricity to keep the plant functioning,” Dr. Ekpenyong added.
Increases in oxygen access and supply can only be achieved by a large and well-coordinated effort. As a result, UNICEF, the Government of Canada, and IHS Nigeria have come together to construct an oxygen plant in Calabar, Cross Rivers State, in the southern part of Nigeria, in an effort to find adequate, long-term solutions.
While the COVID-19 pandemic caused significant disruptions to essential health service delivery, it also highlighted weaknesses in access to medical oxygen and provided opportunities for governments and health system actors to address these gaps. However, strengthening the medical oxygen system is relatively new for program managers, which is why it is critical for UNICEF to continue to strengthen capacity and provide tools such as the Oxygen System Planning Tool to promote a systematic approach to planning, budgeting, implementing, and monitoring progress. This will ensure that adequate and sustainable oxygen supply is available to health facilities, particularly in low-resource settings, to improve patient outcomes and reduce mortality rates associated with critical respiratory and life-threatening illnesses.